
Diabetes affects far more than blood sugar levels. Over time, elevated glucose can quietly damage the small blood vessels throughout your body, and the eyes are especially vulnerable. Many diabetic eye conditions develop gradually, with no pain or noticeable vision changes in the early stages.
That is precisely why routine eye exams matter so much for people living with diabetes. For some patients, a standard annual exam is enough. For others, especially those with fluctuating blood sugar or a longer history of diabetes, more frequent visits may be necessary to catch problems before they affect vision permanently.
How Does Diabetes Affect the Eyes?

High blood sugar creates a cascade of problems inside the eye. When glucose levels remain elevated over months or years, the tiny blood vessels in the retina begin to weaken. Some vessels may swell and leak fluid into surrounding tissue, while others can close off entirely, cutting blood supply to parts of the retina.
These vascular changes set the stage for several serious conditions. Diabetic eye problems include diabetic retinopathy, cataracts, and glaucoma, each of which can lead to permanent vision loss if left undetected. The retina, which converts light into the signals your brain interprets as images, is particularly sensitive to this kind of damage.
What makes these conditions so concerning is how silently they develop. A patient’s vision can seem perfectly normal while significant changes are already taking place inside the eye. By the time symptoms like blurred vision, dark spots, or floaters appear, the damage may be advanced.
What Is Diabetic Retinopathy and Why Does It Progress Silently?
Diabetic retinopathy is the most common eye condition associated with diabetes. It develops when damaged blood vessels in the retina begin to leak or when new, abnormal vessels grow on the retina’s surface.
The condition progresses through two stages. In the earlier stage, called non-proliferative diabetic retinopathy, blood vessels in the retina weaken and may develop small bulges that leak fluid. Many patients have no symptoms at this point. In the advanced stage, called proliferative diabetic retinopathy, the eye attempts to compensate for poor blood flow by growing new blood vessels. These new vessels are fragile and prone to bleeding, which can lead to severe vision loss or retinal detachment.
The silent progression is what makes this condition so dangerous. A patient can move from mild to moderate retinopathy between annual exams without ever feeling a difference. Only a dilated eye exam can reveal these changes in their early stages.
Why Annual Exams May Not Be Enough
For many diabetic patients, yearly eye exams provide adequate monitoring. But certain risk factors can accelerate the rate of change inside the eye, making every-six-month or even quarterly exams a better approach.
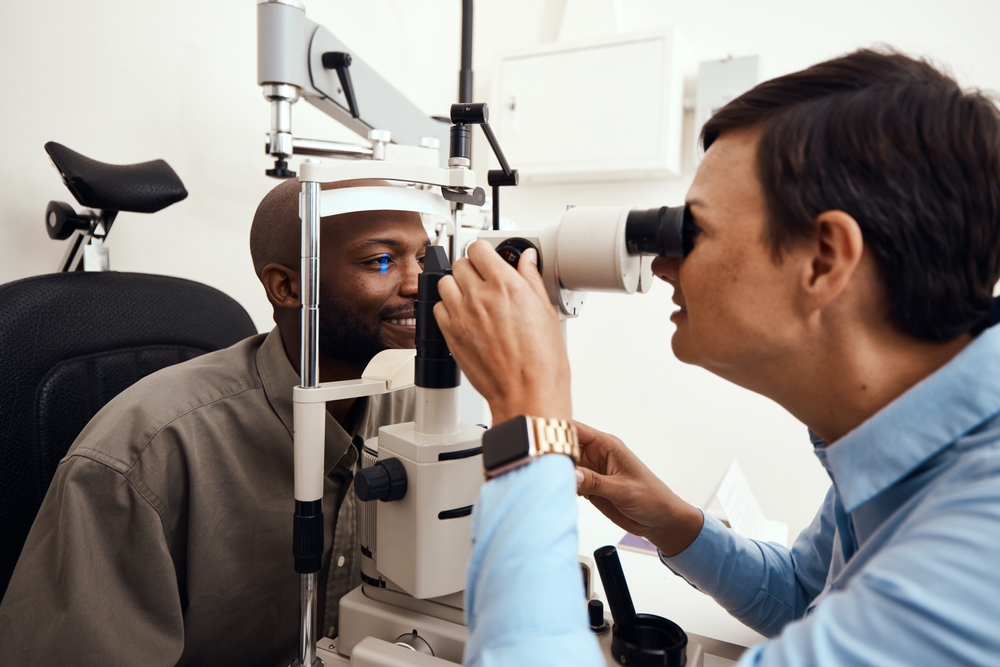
Patients with poorly controlled blood sugar are at the highest risk for rapid progression of retinopathy. Long duration of diabetes (typically ten years or more) also increases the likelihood of eye complications. Other factors that may prompt more frequent exams include:
- High blood pressure or high cholesterol alongside diabetes
- A previous diagnosis of any stage of diabetic retinopathy
- Recent significant changes in blood sugar control
- Pregnancy in a patient with pre-existing diabetes
Your eye doctor can determine the right schedule based on your individual risk profile. The goal is to detect changes early enough to intervene before permanent damage occurs.
Other Eye Conditions Diabetes Can Cause
Diabetic retinopathy gets the most attention, but diabetes also raises the risk of developing cataracts at a younger age. Elevated blood sugar leads to the accumulation of sorbitol in the lens of the eye, which draws in excess water and disrupts the lens’s clarity. This process can cause cataracts to develop earlier and progress faster in people with diabetes compared to those without.
Glaucoma is another concern. People with diabetes are roughly twice as likely to develop open-angle glaucoma, a condition where increased pressure inside the eye gradually damages the optic nerve. Like diabetic retinopathy, glaucoma typically produces no symptoms in its early stages and can only be detected through a comprehensive eye exam that includes tonometry (pressure measurement).
Because these conditions can develop simultaneously, a single exam can screen for multiple threats at once, making regular visits especially efficient for diabetic patients.
What to Expect During a Diabetic Eye Exam
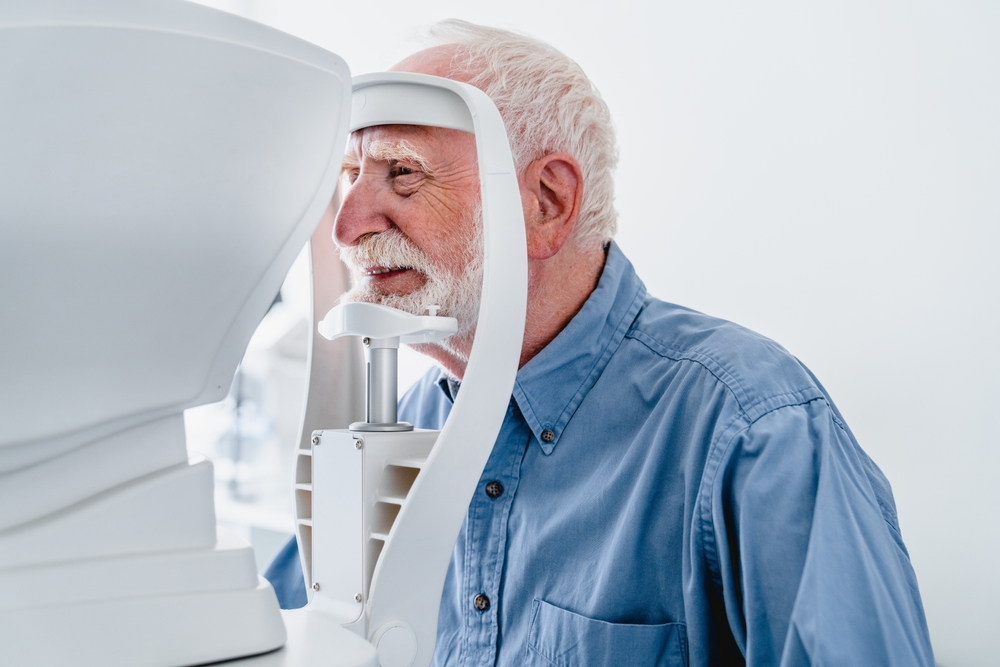
A diabetic eye exam is thorough but straightforward.
It typically begins with a visual acuity test to measure how well you see at various distances. Your eye doctor will then use eye drops to dilate your pupils, which allows a detailed view of the retina, optic nerve, and blood vessels at the back of the eye.
During the dilated portion of the exam, your ophthalmologist will look for signs of leaking or damaged blood vessels, swelling in the macula (the central part of the retina responsible for sharp vision), and any abnormal blood vessel growth. Tonometry, a quick and painless test, measures the pressure inside your eye to screen for glaucoma.
In some cases, your doctor may also use optical coherence tomography (OCT), an imaging technique that captures detailed cross-sectional images of the retina. OCT can detect fluid buildup or subtle structural changes that may not be visible during a standard exam. The dilation drops will cause temporary blurry vision and light sensitivity for a few hours, so bringing sunglasses and arranging a ride home is a good idea.
Protecting Your Vision With Proactive Diabetic Eye Care
The most effective way to protect your eyesight when living with diabetes is to stay ahead of potential problems rather than react to symptoms. Early detection through frequent, comprehensive eye exams gives your doctor the best chance of managing conditions like retinopathy, cataracts, and glaucoma before they threaten your vision.
Due for a diabetic eye exam or concerned about changes in your vision? Schedule an appointment at Eye Specialists of Napa Valley in Napa, CA, today!